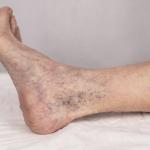
Veins play an important role in circulation by carrying blood back to the heart. In the legs, this process is more complex because blood must travel upward against gravity. When veins are working properly, this system functions efficiently and without noticeable symptoms.
Over time, however, veins may become less effective. Many people begin to notice symptoms such as heaviness, swelling, or visible veins as circulation changes. Understanding why veins stop working properly can help explain how these symptoms develop and why they often become more noticeable with age.
How Healthy Veins Support Circulation
The veins in the legs rely on a combination of one way valves and muscle movement to move blood upward. These valves open to allow blood to flow toward the heart and close to prevent it from flowing backward.
Movement also plays a key role. Each time you walk, the calf muscles contract and help push blood through the veins. This process supports circulation and reduces pressure in the lower legs.
When this system is functioning properly, blood flows efficiently and does not collect in the veins.
What Changes in Veins Over Time
As the body ages, natural changes can affect the structure and function of veins. The walls of the veins may become less flexible, and the valves may weaken over time.
When valves do not close as tightly as they should, blood can begin to move backward instead of continuing upward. This process is known as venous reflux.
As blood pools in the veins, pressure inside the blood vessels increases. This added pressure can cause veins to stretch, enlarge, and become less efficient at moving blood.
People experiencing these changes may notice:
- Legs that feel heavy or tired later in the day
- Swelling around the ankles or lower legs
- Aching or discomfort after standing or sitting
- Visible veins that appear more prominent over time
These symptoms often develop gradually and may become more noticeable as circulation changes continue.
Why Vein Function Naturally Declines
Several factors contribute to the gradual decline in vein function. Aging is one of the most common influences, but it is not the only one.
Over time, repeated pressure on the veins can weaken both the vein walls and the valves. Gravity also plays a constant role, especially in the legs, where blood must be pushed upward throughout the day.
In addition to aging, other factors can increase strain on the veins, including:
- A family history of vein disease
- Jobs that involve long periods of standing or sitting
- Pregnancy, which increases pressure in the veins
- Excess body weight that adds strain to circulation
- Reduced physical activity that limits muscle movement
Because these factors often occur together, their effects can build over time and lead to noticeable changes in circulation.
How Circulation Is Affected by Valve Failure
When vein valves weaken, blood that should move upward toward the heart begins to collect in the lower legs. This leads to increased pressure inside the veins and reduces overall circulation efficiency.
As pressure builds, symptoms such as heaviness, swelling, and fatigue may become more noticeable. In some cases, veins may enlarge and become visible beneath the skin.
This process is a key feature of chronic venous insufficiency, a condition that affects many adults as they age.
How Doctors Evaluate Vein Function
When symptoms suggest a circulation problem, a vein specialist may use a duplex ultrasound exam to evaluate blood flow. This noninvasive imaging test allows doctors to observe how blood moves through the veins and determine whether venous reflux is present.
Ultrasound testing can identify areas where blood is flowing backward or pooling in the veins. This information helps specialists determine the severity of the condition and guide treatment decisions.
Treatment Options That Improve Vein Function
Modern treatments for vein disease focus on improving circulation by closing veins that are no longer functioning properly. Once these veins are treated, blood is redirected to healthier veins that can carry blood more efficiently.
Common treatment options include:
- Endovenous Laser Therapy
- Radiofrequency Ablation
- Ultrasound guided sclerotherapy
These procedures are minimally invasive and are typically performed in outpatient settings with little recovery time.
When to Consider a Vein Evaluation
Changes in vein function often happen gradually, and symptoms may start out mild. However, persistent heaviness, swelling, or visible veins may indicate that circulation is being affected.
A vein specialist can evaluate your symptoms and determine whether vein function has been impacted. Early evaluation can help identify circulation problems and provide options to improve comfort and support long term vein health.
If you notice ongoing changes in how your legs feel or appear, a consultation can help you better understand the cause and explore appropriate next steps.