Varicose veins affect approximately 20% of all adults, which means 1 in 5 people will suffer from them at some point in their lives. The impact varicose veins can have on quality of life can vary greatly from person to person.
For some people, varicose veins may mean nothing more than the unsightly appearance of blue or purple, twisted veins close to the surface of the skin. For others, those same veins may be a sign of compromised circulation in the legs, which, if left untreated, could lead to more problems down the road.
We’ve listed some of the most common signs and symptoms of varicose veins.
What are some signs and symptoms of varicose veins?
If you don’t have any pain:
Some people with varicose veins never have any pain; they have to deal with the cosmetic appearance of the veins. Below are the common signs of varicose veins you’ll deal with even when no pain is involved:
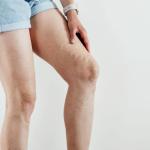
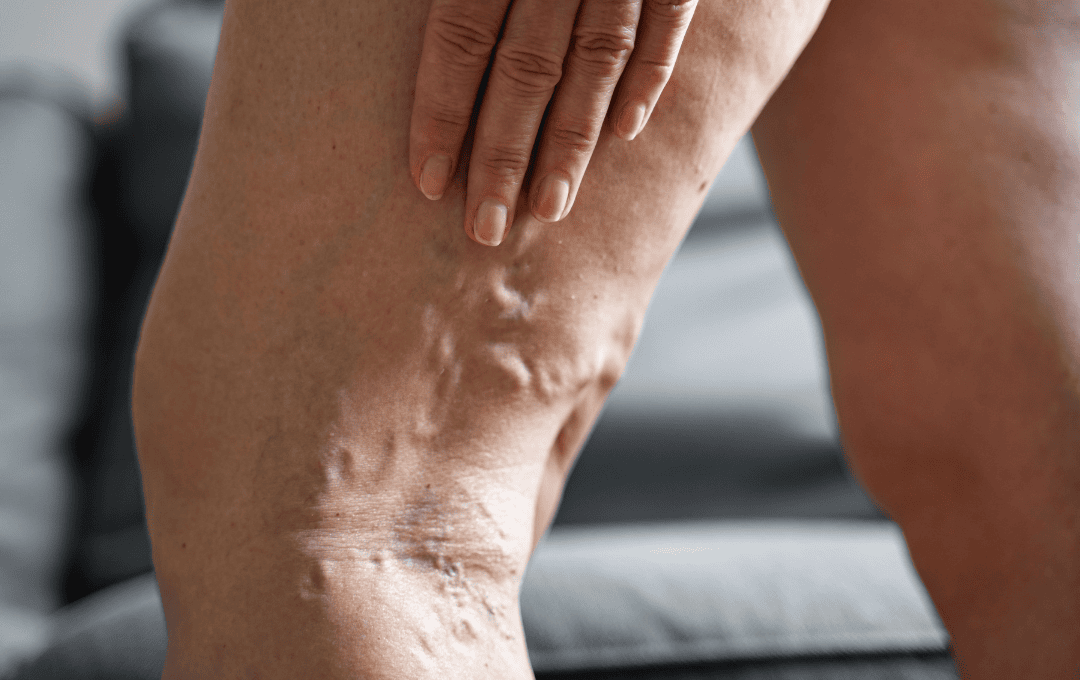
- Veins that appear to be dark purple or blue in color
- Veins that can be bulging and almost look twisted
If you have pain:
Sometimes, varicose veins are not merely a cosmetic issue and come coupled with pain.
Answering the question, “Do varicose veins hurt?” can be tough as the pain level typically varies from person to person. However, here are some common, more painful symptoms of vein disease:
- Burning
- Throbbing
- Muscle cramping
- Swelling
- Aching
- Heavy feeling
- Itchiness around veins
- Skin discoloration around veins
- Increased pain after sitting or standing for long periods of time
Take Our Online Vein Symptoms Quiz
Varicose vein symptoms are typically worse with prolonged sitting, prolonged standing, or at the end of the day. Patients frequently mistake them as a normal part of aging and assume that everyone feels them.
Learn six expert-approved tips for managing varicose vein pain.
If not dealt with, some of these symptoms can get worse and could leave more vein health issues. Let’s get into more detail about the pain associated with these common symptoms.
Skin Discoloration
Stagnant blood pooling at the skin surface in diseased veins can cause chronic inflammation, which in turn results in skin discoloration.
Lipodermatosclerosis
Varicose veins can sometimes mean this condition can cause the skin and the fat under your skin to become inflamed and turn hard. This area of chronic inflammation and scar tissue frequently precedes skin ulceration. If present, lipodermatosclerosis represents an indication to have your veins evaluated and likely treated to prevent ulceration or venous ulcers.
Swelling
Swelling in the legs when you have varicose veins means more than meets the eye. If your legs are swelling, the pressure in your veins has been built up so much that leakage occurs in the tissue around your damaged vein. This will cause great discomfort as it feels like your skin is being stretched tighter and tighter.
Venous Ulcers
According to an article on the National Center for Biotechnology Information, “venous leg ulcers are the most common complication of varicose veins.” If you leave vein issues untreated, “they develop into open wounds about 3 to 6% of the time.”
When blood pools in the veins of the lower legs, fluid and blood cells leak into the skin and other tissues. This causes skin to become itchy and thin, and skin changes called stasis dermatitis. Stasis dermatitis in an early sign of venous insufficiency.
So how do you know if you have venous ulcers? Here are some of the signs and symptoms of venous ulcers you’ll likely encounter:
- Shallow sore with a red base, sometimes covered by yellow tissue
- Sore that is unevenly shaped
- Surrounding skin may be shiny, tight, hot, discolored
- Pain
- May have a bad odor and pus if it becomes infected
If any of these signs or symptoms sound familiar to you, schedule a consultation with one of our vein specialists as soon as possible. Venous ulcers are not things that get better on their own — in fact, they will only continue to get worse.
Deep Vein Thrombosis (DVT)
Something that may start as swelling, pain, tenderness or discoloration in your calf or thigh can be so much more: deep vein thrombosis. Deep vein thrombosis (DVT) is a medical condition that occurs when a blood clot forms in a deep vein. And while you may not be very familiar with that term, DVT is much more common than you’d think. According to the CDC, between 60,000 and 100,000 Americans die every year from DVT and pulmonary embolism (PE), a severe complication of DVT.
So what can you do if your varicose veins hurt and you’re worried that pain may suggest something more serious?
Elevate your legs
Elevate your legs above your heart for short-term relief from pain caused by your veins. This helps the blood flow more easily from your lower body to your heart and takes the pressure off your veins.
Stick your legs in a cold bath
Cold temperatures help shrink swollen blood vessels, which can relieve the heavy feeling you may be experiencing with your varicose veins.
Exercise
Going for a walk or getting moving in any low-impact way will help you regain your blood flow. This is especially important if you are sitting or standing for long periods of time during the day.
Stretch
Stretching is crucial to overall health, but especially to vein health. A few minutes of stretching can relieve struggling veins. Yoga has been known to be a good exercise to help alleviate pain.
Wear compression stockings
Wearing compression socks or stockings during the day may reduce aches and pain associated with varicose veins. Compression stockings help push fluid up the leg, allowing for improved blood flow from the leg to the heart.
Schedule a consultation
No matter what level of pain you are experiencing, the first thing you should do is schedule a consultation with a vein specialist near you. This is the only sure way to determine the true condition of your veins and what level of treatment is required to get your health back on track.
Medically Reviewed By:
Dr. Yan Katsnelson is a philanthropist, business owner, and highly skilled cardiac surgeon. He is the Founder and CEO of USA Vein Clinics, which is part of USA Clinics Group, the parent company of USA Fibroid Centers, USA Vascular Centers, and USA Oncology Centers, with more than 100 facilities nationwide. Dr. Yan has established himself as a strong advocate for accessibility and affordability of the most advanced medical care close to home. His mission is to create a positive experience for each patient with compassionate, personalized, and expert care.