This disorder is something that, a matter of just a few years ago, often went undertreated. The lack of treatment for chronic venous insufficiency can be a result of a few things:
- Lack of technology
- Lack of education/knowledge
- Lack of awareness
However, within the last 10 years, much research has been conducted on this vein disorder that affects a large portion of the population, primarily females.
As a result of that research, awareness has increased and knowledge has been gained. This all has come at a time when technological advances in the medical world are at an all-time high and seem to keep getting better.
Here, we dive into chronic venous insufficiency and how it changes your body, because one of the best ways to put yourself at low risk of developing this disease or avoiding it altogether is to understand what it is and what to look out for.
What is Chronic Venous Insufficiency?
Let’s start with the basics. Chronic venous insufficiency, according to Johns Hopkins Medicine, is something that “occurs when your leg veins don’t allow blood to flow back up to your heart.”
They go on to say that “normally, the valves in your veins make sure that blood flows toward your heart. However, when these valves fail to function properly, blood can also flow backward. This can cause blood to collect (pool) in your legs.”
What Causes Chronic Venous Insufficiency?
Like most vein problems, there are several reasons a person may develop vein issues, such as chronic venous insufficiency.
The top reasons for developing chronic venous insufficiency include:
Obesity
Obesity puts people at risk of developing several health problems. Heart issues steal the spotlight, and most people do not think about the fact that obesity can wreak havoc on your veins, too.
The amount of weight and pressure that your veins fall victim to when you’re obese makes it difficult for them to function normally. Your veins are unable to return blood through your body back to your heart as they normally do, which leaves the blood to pool in your legs and other areas as well.
Hormone changes (including menopause and pregnancy)
Changes in hormones are another major risk factor for venous insufficiency. The most common time to experience these hormonal shifts is during pregnancy.
Unfortunately, with each pregnancy, your chances of having vein issues increase. There is a great deal more pressure put on your veins when you are pregnant, so chances are higher that you may find yourself suffering from weakened or damaged veins.
Age
Specifically, over the age of 50. Unfortunately, it is just part of aging that your veins will weaken over time. Think about it — they have been used more than, say, a 20-year-old’s veins, so they don’t have the strength that the veins of someone younger do.
Thus, the older you are, the more at risk you are of developing venous insufficiency due to the weakening of your veins and the increased struggle for your veins to return blood to your heart.
Genetics
Unfortunately, you can’t fight your genes. Some people can have a genetic predisposition to develop vein issues, and there is just no way around it.
You can help make your venous insufficiency issues less severe if you know ahead of time that you are at a higher risk for problems, and do your best to step up your health in other areas of your life.
Sedentary lifestyle
One of the biggest risk factors for chronic venous insufficiency is the lack of body movement. Sitting or standing too much is horrific for your overall health, but for your veins in particular. The longer you stay in one place (whether that’s standing or sitting), the harder it is for your body to pump your blood properly.
Because your veins are fighting against gravity to pump blood back up to your heart, it’s important you help out a bit and get moving so that your veins don’t have to work at their maximum all the time.
Another reason a sedentary life is risky for your vein health is that the more sedentary you are, the more likely you are to experience weight gain. As mentioned above, weight gain is not beneficial for your veins.
Smoking
Like a number of the things mentioned above, smoking does damage to your health in some ways, including something most people don’t think about — yep, you guessed it: your veins. Smoking leads to the weakening of your veins’ walls, which means you are at a higher risk of venous insufficiency.
You have to keep those lungs and those vein walls strong!
How Do I Know if I Have CVI?
The only way to be 100% sure that what you have is indeed chronic venous insufficiency, you would need to schedule a consultation with a vein specialist.
If you do have chronic venous insufficiency, here are some things you’ll notice.
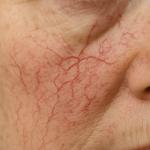
The most common change you will experience is dilated veins. Your veins will widen with this disorder and will appear as either spider veins — blue, thin veins — or varicose veins — wider veins on the surface.
Swelling is also a common symptom associated with chronic venous insufficiency. This swelling can occur throughout the day or simply at the end of the day when you finally give your legs a rest. However, note that swelling is most often at its lowest intensity in the morning, due to the fact that elevating your legs (as you do while sleeping), causes swelling to go down.
The change in the color of your legs is something you can also expect. This happens because weakened veins cause the blood in your legs to pool, which then causes your skin to become inflamed. This inflammation can take the form of:
- Itchiness
- Dryness
- Open sores
- Redness
- Fluid oozing
- Hard, shiny areas
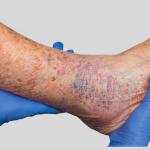
And, ulcers, they don’t sound pretty, and sure aren’t pretty either. These ulcers are most commonly found on the ankle but sometimes occur on the shin as well.
These ulcers are essentially sores that are open, and will not heal for months, possibly even years. They are painful and certainly uncomfortable and have been known to ooze fluid often.
How Can I Treat Chronic Venous Insufficiency?
If you’re faced with chronic venous insufficiency, chances are good you’re curious how you can treat it. Well, on your own, the best way to handle this disorder is to do what you can to lessen the severity of the symptoms.
Here are some things you can try to help treat chronic venous insufficiency:
Elevating your legs
With just 30 minutes a few times a day of elevating, you’ll find a decrease in the swelling of your legs and see your blood flow improve.
By elevating your legs, you can help improve your venous ulcers. People with mild chronic venous insufficiency find that elevating their legs may be all the treatment they need, while people who suffer from a more severe form of the disorder may need additional treatment.
Compression stockings
Depending on the severity of your chronic venous insufficiency, you may be able to get stockings just over the counter at the drugstore. If your disorder is more serious, you’ll need prescription-level stockings.
These stockings work to compress your leg, allowing your blood flow to improve and flow more smoothly, thereby avoiding pooling.
Sclerotherapy
This is for more serious cases of chronic venous insufficiency, but don’t worry — it is not major surgery. At USA Vein Clinics, we perform sclerotherapy on a regular basis, and our patients have incredible success with it.
Sclerotherapy involves injecting the vein with something that causes it to collapse. While the damaged vein remains in your leg, it is no longer responsible for carrying your blood, so it will no longer suffer and cause you trouble.