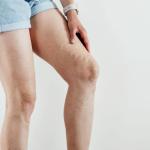
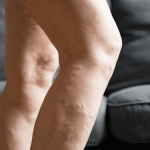
Vulvar varicosities, also known as vulvar varices, are varicose veins that affect the vulva, labia minora and/or labia majora, which is the external part of a woman’s genitals. While not as common as other types of varicose veins, vulvar varicosities occur in roughly 4% of women (source). These also occur in an estimated 22%–34% of women with varicose veins of the pelvis and in 18%–22% of pregnant women. During the postpartum period, perineal veins may persist and enlarge with time in 4% – 8% of patients (source).
Vulvar Varicosities During Pregnancy
The most common contributor to vulvar varicosities is pregnancy. In other posts, we have discussed how pregnancy can lead to varicose veins in your legs and how to treat varicose veins while pregnant. Unsurprisingly, it is those same factors that lead to vulvar varicosities during pregnancy.
Book a Consultation with a Vein Specialist Near You
Common Causes of Vulvar Varicosities
So what exactly causes vulvar varicosities? Read below to discover the most common causes of vulvar varicosities in women.
Increase in blood volume
As a baby grows, the blood volume needed to supply that baby also grows. In fact, women’s blood volume during pregnancy increases anywhere from 30-100%, averaging at a 45% increase (source).
Hormones
Progesterone allows our vessel to stretch to compensate for additional blood flow. Sometimes when veins are stretched during pregnancy, they don’t retract to their prior size, allowing for venous flow to move the wrong direction, creating bulging varicose veins, and/or spider veins.
Pressure
As you can imagine, additional blood volume combined with where the baby sits, moves or even kicks, causes increased pressure on the veins in the pelvis. Towards the end of the third trimester, your body continues to work against gravity to move the blood out of your legs and back towards your heart and lungs. Also, as the baby grows, so does the uterus. Your abdomen experiences additional pressure, potentially obstructing or partially obstructing the veins that pass through your pelvis as well as your legs.
This additional pressure causes the veins to stretch further, making it more difficult for them to reduce to normal size postpartum. This can lead to failing valves in your veins, causing spider veins, varicose veins, and vulvar varicosities.
Multiparity
Each subsequent pregnancy leads to the cycle of additional blood volume, hormone changes and additional pelvic pressure, making it more difficult for veins to return to their normal size and elasticity. As the pelvic veins continue to stretch out with each pregnancy, the valves in the veins may no longer touch allowing venous flow to move in the wrong direction. This leads to varicose vein disease which can affect the pelvis and legs.
Do You Have Vulvar Varicosities But You’re Not Pregnant?
Although pregnancy is the most common cause of vulvar varicosities, other risk factors exist which may predispose some women to this venous disease process, including:
- Genetics: While the exact reason is not yet fully understood, if a parent, grand parent, or even great grandparent had varicose veins, you are at a higher risk for varicose veins as well. This includes vulvar varicosities.
- Pelvic Venous Disorders: Formerly known as Pelvic Congestion Syndrome, pelvic venous disorders occur when the veins in the pelvis are unable to properly move the blood out of pelvis, over time, causing the veins to stretch, twist and hold additional venous blood. While this disease process is most commonly caused by multiparity, it can also occur in women who have never been pregnant due to an increase in pressure in the veins of the pelvis.
- Obesity: Those with a body mass index (BMI) of 30 or greater are predisposed to varicose vein disease due to the additional pressure on venous flow.
Signs and Symptoms of Vulvar Varicosities
Just like varicose veins in the legs, you can have signs of vulvar varicosities but no symptoms, symptoms but no signs, or both signs and symptoms. Remember: Signs are the visible signs that may present themselves on your body, while symptoms are the physical symptoms that you may feel. So, what should you look for?
Take Our Online Vein Symptoms Quiz
Visual Digns of Vulvar Varicosities Include:
- Bulging, twisted, swollen, or clustered veins just beneath the skin which are most apparent when standing
- Veins can be blue, purple, or skin color with bulging veins that appear blue or purple in color underneath your skin
- These veins can appear on your vulva, upper thigh, inner seam of your leg, or near the buttocks
Physical Symptoms You May Feel Include:
- Fullness, pressure, discomfort, or pain in or near your vulva
- Itchiness
- Pain or discomfort in your upper thighs and lower back
- Pain or discomfort that gets worse during or after intercourse
- Pain while walking or when standing too long
In general, vulvar varicosities can be uncomfortable, but not dangerous, however, be sure to visit a vein specialist right away if your vulvar varicosities become:
- Red
- Hard
- Swollen
- Painful
Vulvar Varicosities Treatment Options
The good news is, if you suffer from vulvar varicosities, you are not alone! Vulvar varicosities are not uncommon, and treatments are therefore usually covered by most major insurance providers. Treatment plans are unique to each patient and based on a physical exam as well as an ultrasound and/or other imaging modality findings.
At-Home Treatment for Vulvar Varicosities
While it won’t rid you of your vulvar varicosities, these at home options may provide temporary relief:
- Lying down and propping your hips up to help the venous flow
- Changing positions regularly
- Wearing graduated compression stockings
- Taking NSAIDS*
- Icing the affected area(s)
- Using a topical corticosteroid cream to relieve itching*
*Remember to always consult a physician prior to taking any medication or using ointment.
Seeking Relief From Your Vulvar Varicosities Symptoms
If you are worried about your symptoms, varicosities, or are experiencing discomfort, seek the advice of a vein specialist who can provide you with a customized vein treatment plan. Treatment options for vulvar varicosities include:
- Phlebectomy: Phlebectomy removes the affected veins, requiring a few small incisions made on the skin’s surface.
- Transcatheter embolization: This treatment utilizes fluoroscopic imaging, a type of X-ray, to help your doctor guide a catheter into the varicose vein. Your doctor then places a coil or sclerotherapy solution to close off the vein.
- Sclerotherapy: Sclerotherapy is one of the more common ways to treat vulvar varicosities. In this procedure, your physician injects a medication (sclerosant) directly into the veins, causing them to shut down.
Learn more about our minimally invasive approach to vein treatment.
Vulvar varicosities can significantly affect your quality of life but are not uncommon and can easily be treated. If you are experiencing discomfort physically or emotionally due to your vulvar varicosities, why wait? Prioritize yourself and make the decision to discuss your vein health with a vein specialist today.
You don’t have to suffer from vulvar varicosities! Book a consultation with USA Vein Clinics today and take the first step towards a better tomorrow.